OCTOBER is Breast Cancer Awareness Month

Call to Book a Screening in Nova Scotia:
1-800-565-0548 or (902) 473-3960
Please have your Nova Scotia Health Card ready!
What is Breast Cancer?
Breast cancer occurs when breast cells begin to grow and divide at an uncontrolled pace. Normal breast cells grow and divide as needed and then die as they age or suffer damage. In contrast, breast cancer cells continue to divide, resist cell death signals, and gain capacity to invade, eventually forming masses called tumours. A cancerous (malignant) tumour is a group of cancer cells that can grow into and destroy nearby tissue. It can also spread (metastasize) to other parts of the body.
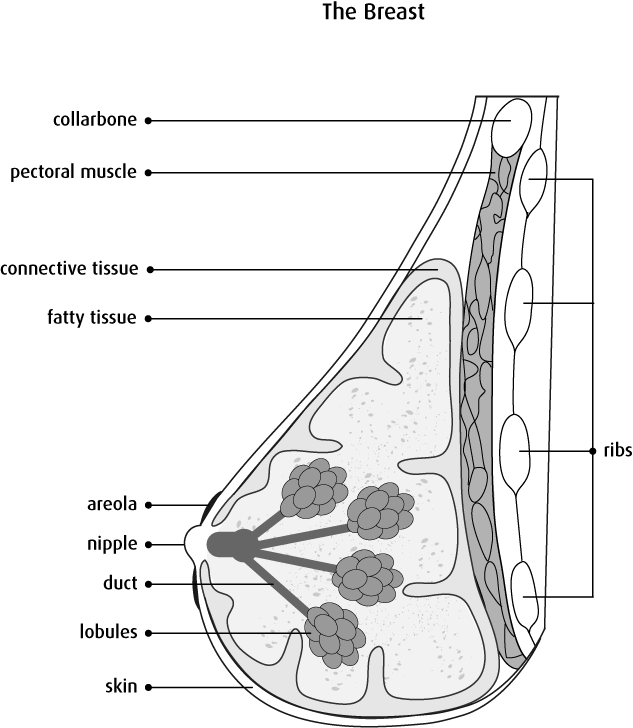
Typically, breast cancer begins either in the cells of the ducts—this is called ductal carcinoma—(the channels that carry milk from the glands to the nipple) or the lobules—this is called lobular carcinoma—(the groups of glands that create milk). Both types of carcinoma can be in situ or invasive. In situ means that the cancer is in its original place and has not invaded into the nearby tissues. Invasive means cancer has spread from where it began into the surrounding healthy tissues.
Less common types of breast cancer can also develop. These include inflammatory breast cancer, Paget disease of the breast and triple-negative breast cancer. Rare types of breast cancer include non-Hodgkin lymphoma and soft tissue sarcoma.
Quick Stats on Breast Cancer
In Canada:
- 1 in 8 Canadian women will be diagnosed with breast cancer in their lifetime.
- It is the second leading cause of death from cancer in Canadian women (it can occur in men but it is not common).
- Thanks to early detection and new treatments, the 5-year survival rate is 87%.
For women in Nova Scotia, breast cancer is the most frequently diagnosed type of cancer.
In 2019, an estimated:
- 800 women will be diagnosed with breast cancer.
- 160 women will die of breast cancer.
Risk Factors
There is no single cause of breast cancer but some factors that increase the risk of developing the disease include:
- Age: 82% of the cases of breast cancer occur in women over 50 years of age.
- Personal History: if you have previously had breast cancer.
- Family history: especially in a mother, sister or daughter diagnosed with breast cancer before menopause, or if a mutation on the BRCA1 or BRCA2 genes is present.
- Previous breast disorders: breast disorders with biopsies showing abnormal cells.
- Pregnancy: no full-term pregnancies or have a full-term first pregnancy after age 30.
- Menopause: obesity and physical inactivity in post-menopausal women; later than average menopause.
- Menstruation: beginning to menstruate at an early age (11 or younger).
- Medication: taking hormone replacement therapy (estrogen plus progestin) for more than 5 years.
- Smoking: the effects of smoking and never breastfeeding are currently under study.
- Alcohol - Even low levels of alcohol consumption (just over one drink per day) can increase a woman’s risk. The risk increases with the amount of alcohol consumed.
Many risk factors are modifiable, to learn more about reducing your risk please CLICK HERE. For more details on the risks, CLICK HERE.
Signs/Symptoms
The most common symptom of ductal carcinoma is a firm or hard lump that feels very different from the rest of the breast. It may feel like it is attached to the skin or the surrounding breast tissue. The lump doesn't get smaller or come and go with your period. It may be tender, but it's usually not painful (pain is more often a symptom of a non-cancerous condition).
Lobular carcinoma often does not form a lump. It feels more like the tissue in the breast is getting thicker or harder. Other symptoms of ductal and lobular breast cancer include:
- a lump in the armpit (called the axilla)
- changes in the shape or size of the breast
- changes to the nipple, such as a nipple that suddenly starts to point inward (called an inverted nipple)
- discharge that comes of the nipple without squeezing it or that has blood in it
- dimpling or puckering of the skin of the breast
- redness, scaling or inflammation of the nipple
- the breast becomes red, swollen or hot
Please see a doctor if you experience any of these signs or symptoms! Your doctor may then refer you for a mammogram. Remember, 80% to 90% of breast lumps are not cancer.
Screening
For information on screening in Nova Scotia, please CLICK HERE.
What is a mammogram?
Mammograms are x-rays of the breasts. A screening mammogram looks for an unsuspected, hidden cancer in women who are healthy and who have never had breast cancer.
Who should get a mammogram?
The Canadian Association of Radiologists (CAR), National Standards and Guidelines for Breast Screening, recommend mammography screening for asymptomatic women at least 40 years of age as well as:
- no new breast symptoms
- no breast implants
- no personal history of breast cancer
- minimum of one year since the previous mammogram
- a resident of Nova Scotia with a valid Nova Scotia health card
How often should you have a mammogram?
Women in Nova Scotia, aged 40-49, are recommended to have annual screening mammography.
Women in Nova Scotia, aged 50-74, are recommended to have screening mammography at two-year intervals. Women 50-74 can also be recommended to return on an annual basis if they:
- have a strong family history of breast cancer (mother, sister, daughter, father, brother, son)
- are currently on HRT
- the radiologist has recommended returning sooner
Women over the age of 75 are recommended to continue to have screening mammography if they are in good health.

Treatments
If you have breast cancer, your healthcare team will create a treatment plan just for you. It will be based on your health and specific information about cancer. When deciding which treatments to offer for ductal carcinoma and lobular carcinoma, your healthcare team will consider:
- the stage
- if you have reached menopause
- the hormone receptor status of the cancer
- the HER2 status of the cancer
- the risk that the cancer will come back, or recur (for early-stage breast cancers)
- your overall health
You may be offered one or more of the following treatments for breast cancer:
Surgery
Most women with breast cancer will have surgery. Your healthcare team will talk to you about the different types of surgery to help you decide which is best for you. The types of surgery you will be offered depend mainly on:
- the size and location of the tumour
- the size of the breast
- if the cancer has spread to the lymph nodes
- if you have already had any treatments for breast cancer
Surgery for breast cancer includes breast-conserving surgery, mastectomy and lymph node surgeries.
Radiation therapy
External beam radiation therapy uses a machine to direct radiation through the skin to the tumour and tissue around it. Radiation therapy is almost always given after breast-conserving surgery. In some cases, it may be given after a mastectomy. It is also used to treat breast cancer that has spread to the bones, lungs or brain.
Hormonal therapy
Hormonal therapy is often used to treat hormone receptor-positive breast cancer. Post-menopausal women are given different hormonal therapy drugs than premenopausal women.
Chemotherapy
Chemotherapy is a common treatment for breast cancer. It is often given after surgery for early-stage breast cancer to reduce the risk that the cancer will come back. It is also the main treatment for advanced or metastatic breast cancer.
Targeted therapy
Targeted therapy may be given alone or in combination with chemotherapy, hormonal therapy or both.
Websites to visit for more information:
Nova Scotia Breast Screening Program
Public Health Agency of Canada information about Breast Cancer
